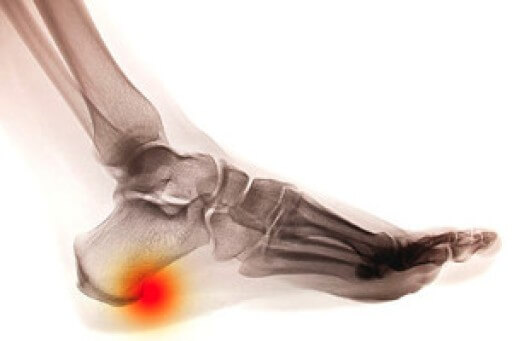
As small as a heel spur is, it can bring severe pain and discomfort to the patient. It is a bony protrusion that may be pointed and is found underneath the heel. It is a calcium build-up, and can gradually come from wearing shoes that do not fit correctly. Many times a heel spur may be misdiagnosed as plantar fasciitis, which is another condition that affects the heel. A diagnosis consists of undergoing an examination that can determine how tender the heel is, in addition to possibly having an X-ray taken. There are patients who find mild relief when anti-inflammatory medications are taken, despite being a temporary fix. Another option that may be considered are custom-made orthotics, and these may help to diminish pressure on the Achilles tendon. If you have heel pain, it is strongly suggested that a podiatrist is consulted who can determine what the cause is, and offer correct treatment options.
Heel spurs can be incredibly painful and sometimes may make you unable to participate in physical activities. To get medical care for your heel spurs, contact the podiatrists from Boston Common Podiatry. Our doctors will do everything possible to treat your condition.
Heels Spurs
Heel spurs are formed by calcium deposits on the back of the foot where the heel is. This can also be caused by small fragments of bone breaking off one section of the foot, attaching onto the back of the foot. Heel spurs can also be bone growth on the back of the foot and may grow in the direction of the arch of the foot.
Older individuals usually suffer from heel spurs and pain sometimes intensifies with age. One of the main condition's spurs are related to is plantar fasciitis.
Pain
The pain associated with spurs is often because of weight placed on the feet. When someone is walking, their entire weight is concentrated on the feet. Bone spurs then have the tendency to affect other bones and tissues around the foot. As the pain continues, the feet will become tender and sensitive over time.
Treatments
There are many ways to treat heel spurs. If one is suffering from heel spurs in conjunction with pain, there are several methods for healing. Medication, surgery, and herbal care are some options.
If you have any questions feel free to contact our office located in Boston, MA . We offer the latest in diagnostic and treatment technology to meet your needs.